|
The CLO view is equally efficacious in the lumbar epidural space because of its precision and superior needle visibility and trajectory however, there are a few important differences. Differences Between Cervical and Lumbar Access Physicians should familiarize themselves with those patterns yet recognize that despite the pattern, the dorsal margin of the contrast approaches the ventral margin of the lamina in the CLO view and subarachnoid or other spread must be considered when it is not observed. 2D: Lower-intensity contralateral spread appears as only a thin film in the X-ray path.Ī multitude of epidural contrast spread patterns may be seen in the contralateral view (eg, thick, thin, nerve root spread, multi-intense, vacuolations) depending on location of spread (eg, ipsilateral, contralateral, bilateral), and epidural distention may also occur (Figure 2). The needle is advanced beyond the ventral interlaminar line before resistance is lost. 2C: In the lumbar spine ligamentum flavum (outlined), hypertrophy has a typical appearance. 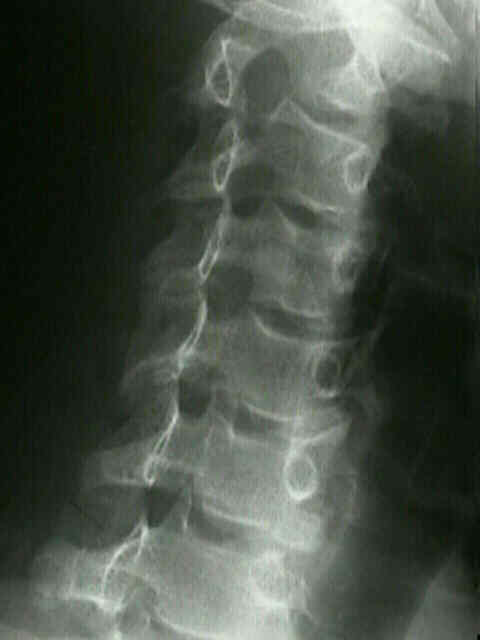
Intradural spread may also appear like this. 2B: A thick pattern may represent midline pooling or epidural space distension with restricted spread. 2A: Contralateral vacuolation is observed in this typical spread. Loss of resistance can be subtle or nonexistent, especially with thin gauge needles.įigure 2: Contralateral oblique view contrast spread patterns. Do not advance more than 2.5 mm beyond the VILL. Expect to lose resistance at or within 2 mm of the VILL (Figure 1).Advance the needle to just before the VILL in anteroposterior (AP) and CLO views.Confirm correct needle trajectory, identify the ventral laminar margin and conceptualized ventral interlaminar line, and estimate the distance to the VILL (Figure 1).For midline needle approaches, either direction may be used. The image intensifier obliquity is opposite to the side where the needle is inserted. This may be a few centimeters, depending on the patient. Advance the needle until it engages in firm tissue.Infiltrate with local anesthetic, making sure that the skin does not translate.A needle insertion point below the laminar edge provides an additional safety margin and improved needle trajectory. Remain within the lateral margin of the spinous process to prevent inserting the needle too lateral. Mark the insertion point on the correct side.Identify the laterality of pain symptoms.Open the interlaminar space (may require cephalad tilt of the fluoroscope).Identify the correct cervical vertebral level (not higher than C6–C7).Position the patient prone with their neck slightly flexed and forehead on a pillow.Step-by-Step Cervical and Cervicothoracic Epidural Access Its advantages extend to the lumbar spine as well, with demonstrated superiority in visualization and precision. These advantages make the CLO view a clear favorite both for ease of access and for precision, likely enhancing overall safety of fluoroscopic epidural access. The needle trajectory can be clearly projected (Figure 1). Thus, the needle can be placed directly within 1–2 mm of the target and the epidural space can be immediately accessed. 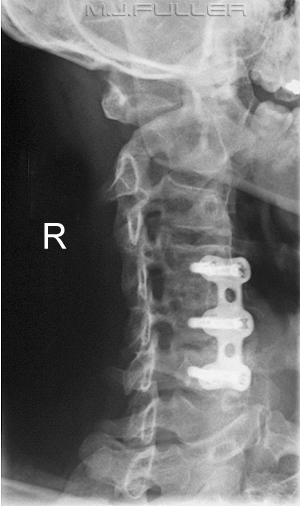
The needle tip is always well visualized and the relationship of the posterior boundary of the epidural space to the ventral inter-laminar line (VILL) is very tight (Figure 1). The contralateral oblique (CLO) view, on the other hand, affords both. The needle tip is often poorly visualized or may not be visualized at all, and the spinolaminar junction is an inadequate radiologic landmark for the depth of the epidural space because of great variability. 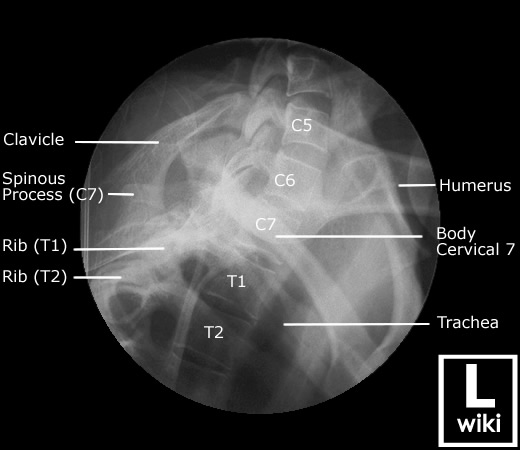
The commonly used depth view for fluoroscopic epidural access, the lateral view of the spine, affords neither. Because the distance from the epidural space to the spinal cord is diminutive, the depth of the needle as it approaches the cervical epidural space must be continually monitored and a radiologic landmark must serve as a depth marker for the epidural space. The likely primary driver is ineffective use of fluoroscopy however, even more likely is the limitation of fluoroscopy itself. “The CLO view is a clear favorite both for ease of access and for precision, likely enhancing overall safety of fluoroscopic epidural access.” An American Society of Anesthesiologists closed claims analysis for cervical procedures performed from 2005–2008 found 20 reported cases of direct spinal cord injury during interlaminar cervical epidural access. Safety is of particular importance when performing procedures involving the cervical spine, and therefore accuracy with needle placement is critical. Fluoroscopic epidural access, whether for an epidural steroid injection or for spinal cord stimulator lead insertion, is one of the most common procedures in the field of pain medicine.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
